-------------------------------------
Screwworm is here, World Cup starting, things heating up (literally), and more.
Katelyn Jetelina, The Dose, 6-9-26
Movement is the name of the game this week: people, animals, insects, and the health impacts that follow.
The World Cup kicks off Thursday, pulling millions together in celebration, but where crowds gather, pathogens follow. We’re debuting a new section on the health signals worth watching. Also on the move: a parasitic, flesh-eating fly eradicated in the U.S. in 1966 has found its way back (yes, it’s as terrible as it sounds). And 48 million people are facing serious heat risk. Good news is in the mix, too.
Here’s what’s going on, and most importantly, what it means for you.
Health “weather” report
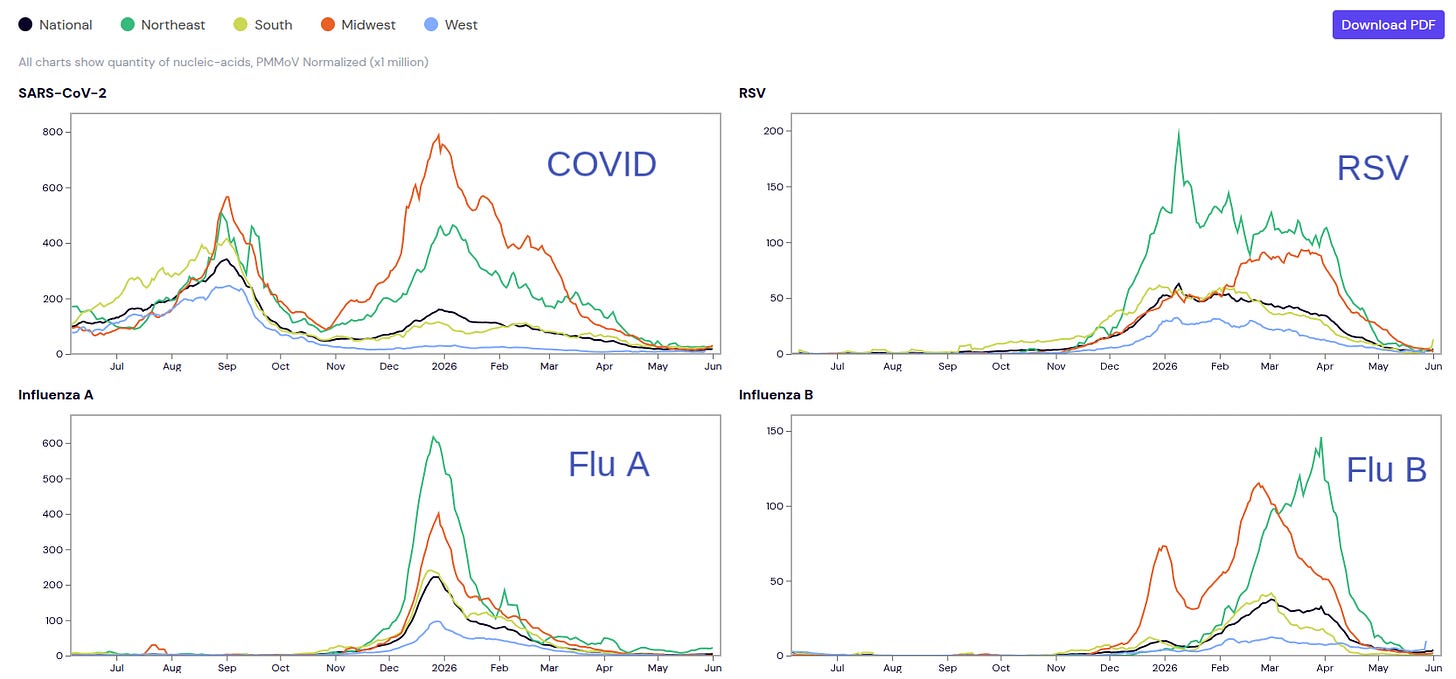
Ticks are still increasing, and all respiratory diseases are declining to very low levels.
Things are heating up
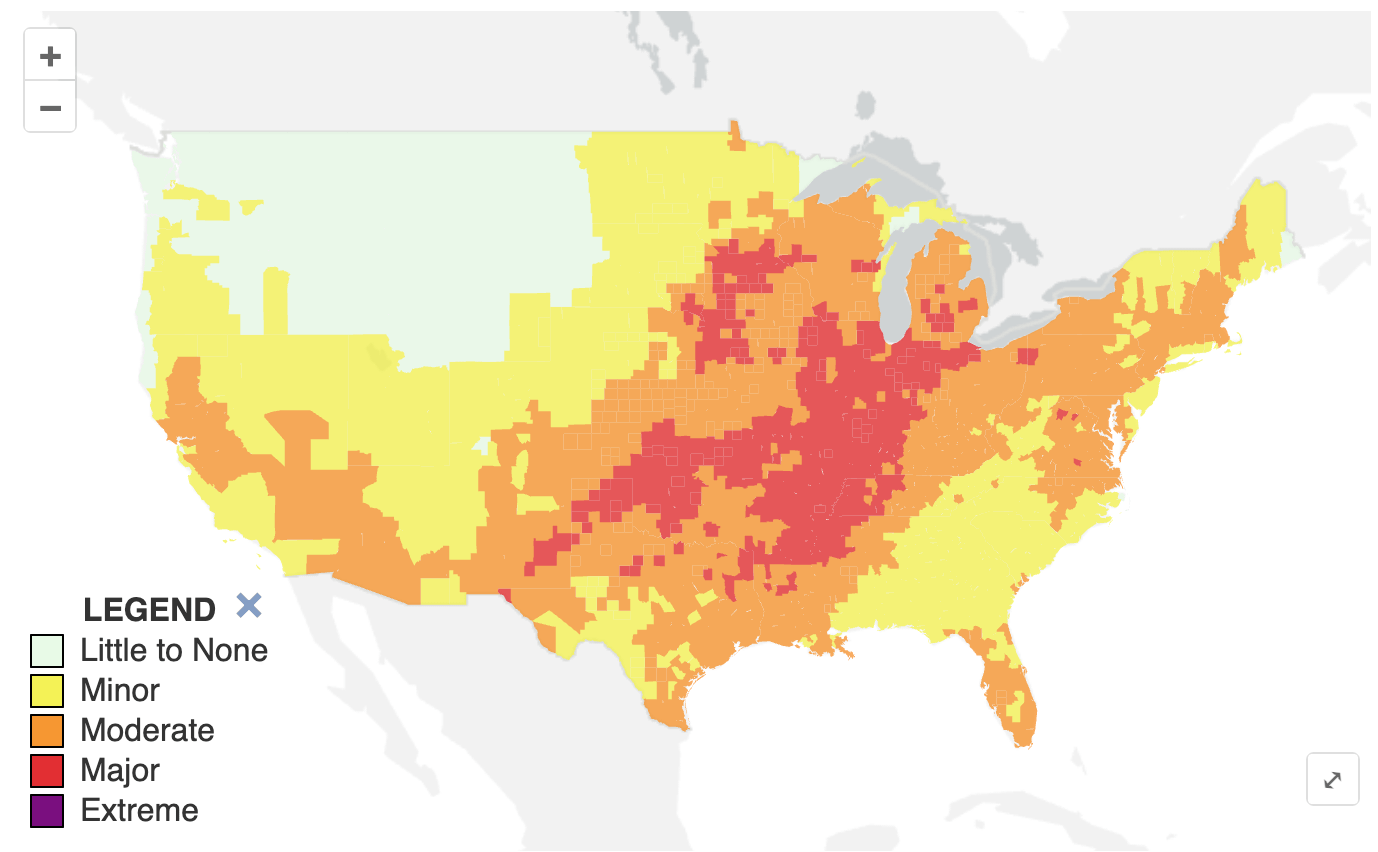
This week, 48 million people will face “major” heat risk, and 100,000 will face “extreme” heat risk.
When it comes to extreme heat, it’s not just about the temperature you see on your weather app. While 120 degrees in Phoenix isn’t great, 90 degrees in New York can be worse.
This is because the risk to your health is due to heat imbalance. That’s when your body produces more heat than it can release. Normally, sweat helps cool us down. But when it’s hot and humid, sweat doesn’t evaporate as easily. The air is already packed with moisture, making it harder for your body to cool itself and raising the risk of illness quickly.
What this means for you: The following people should take action when their area is “orange” or higher. Everyone else, start taking action in “red.”
People taking medications that impair heat regulation: Certain drugs interfere with sweating, hydration, or heart function, and can even reduce your thirst sensation. Check out the list here.
Older adults: Aging reduces the body’s ability to sweat and regulate temperature.
Infants and children: Smaller bodies heat up faster, and young children may not recognize or communicate early symptoms. Kids with asthma are at high risk.
People with chronic diseases: Underlying conditions like heart disease strain the body’s ability to cope with heat stress.
Pregnant women: Pregnancy increases metabolic heat production, making it harder to stay cool. More here.
Outdoor workers and athletes: Prolonged physical activity in hot environments increases internal heat production.
People experiencing homelessness: Continuous exposure to heat, dehydration risk, and limited access to cooling or hydration increases vulnerability.
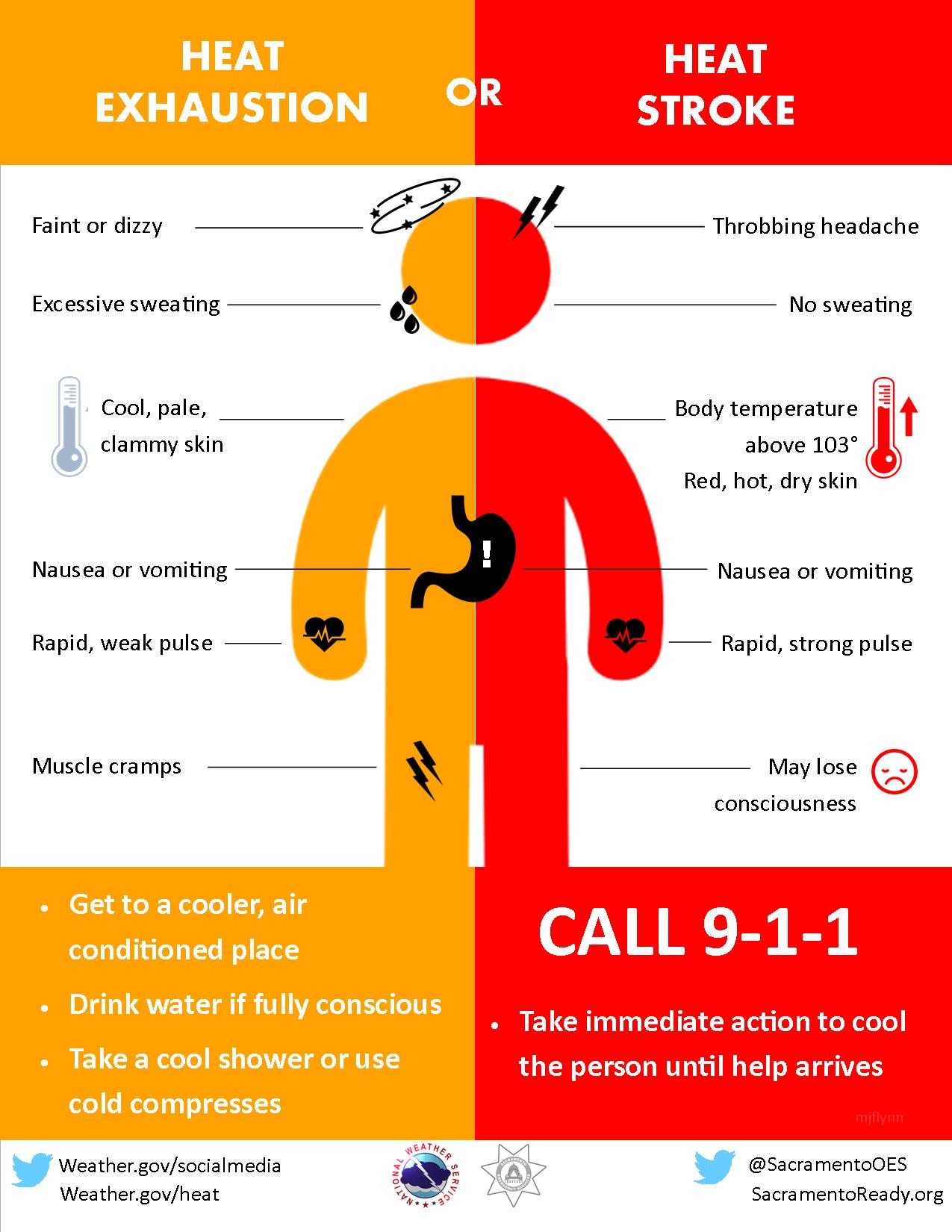
Check the HeatRisk tool to know when to avoid strenuous activity. Stay hydrated. Watch for signs and symptoms of heat stroke. Check your urine color.
Be smart with fans: Fans can help when it’s moderately hot by circulating air and helping sweat evaporate. But once temps climb above 90°F fans may actually blow more hot air onto you, increasing heat stress.
Healthy Cup: Let the games begin!
The World Cup officially kicks off Thursday! YLE is playing a key role at the national Health Security Operations Center, and each week, we’ll share what we’re seeing in the data for those heading to the games or simply curious about what happens when millions of people mix.
While we wait for the games to start, epidemiologists are watching signals at and around base camps and practice games this past week.
The risk remains low, but three signals are garnering attention for now:
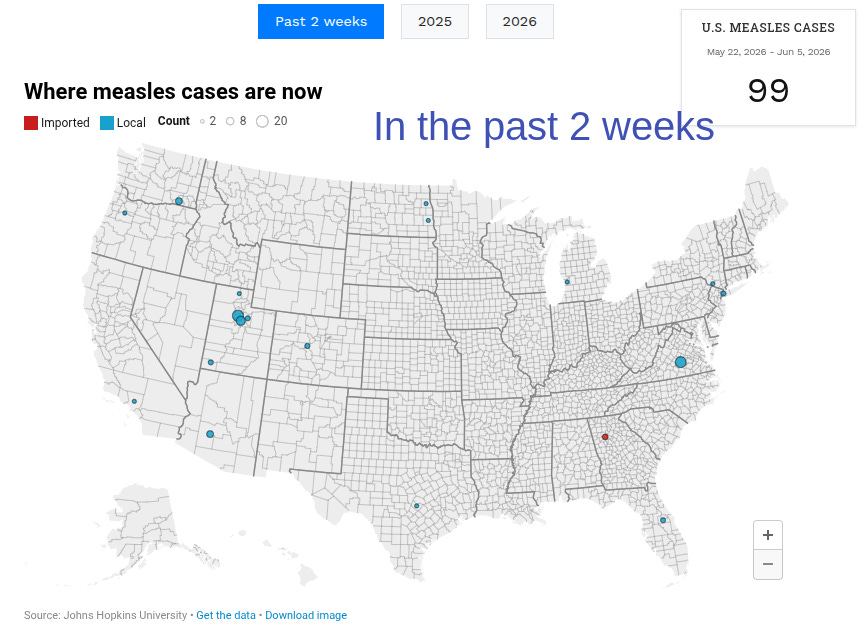
Measles continues to spread in all three host countries, with a significant ongoing outbreak in Mexico. Seven base camps and practice games are near outbreaks, and these teams and their fans will soon disperse to other locations for the tournament. Make sure you’re up to date on the MMR vaccine and protection.
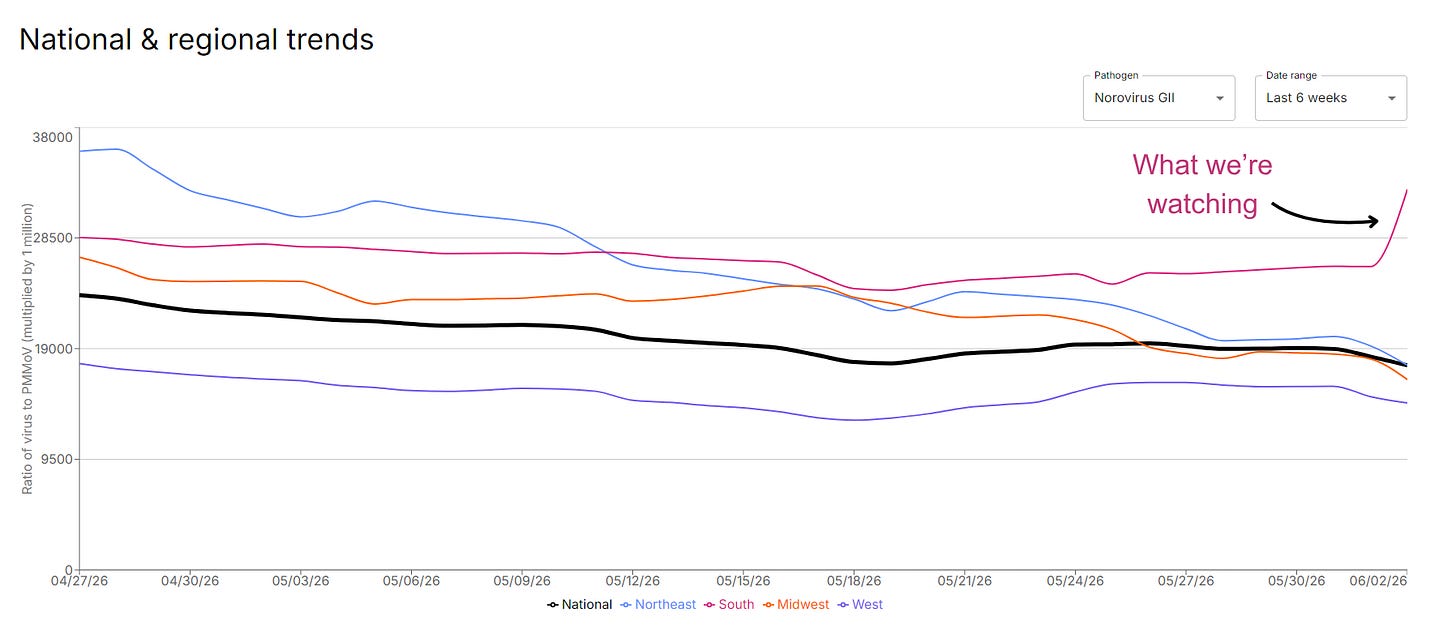
Norovirus (nausea, vomiting, diarrhea) is declining nationally, with one notable exception: a sharp increase in the South that’s unusual for this time of year and worth watching. This is very contagious, and hand sanitizer won’t work. Wash your hands with soap and water.
On heat… There was significant public concern about FIFA banning water bottles, which could become a big deal for heat-related illnesses. But on Friday, FIFA clarified (or walked back) its policy, saying attendees are allowed one 20-ounce (591 mL) unopened, soft-plastic disposable bottle (think: a bottle from a vending machine). Drink up.
We will be back next week for more.
Spotlight: Screwworm. The fly has landed.
Five cases of New World screwworm have been confirmed in the U.S. Texas declared an emergency, and Canada immediately restricted livestock imports. This bug could quickly turn into a big deal, and scientists have long warned about its return (I am surprised it didn’t come sooner, to be honest).
I called arbovirologist Dr. Miguel Arturo Saldaña in Texas to help break it down.
Screw… what?
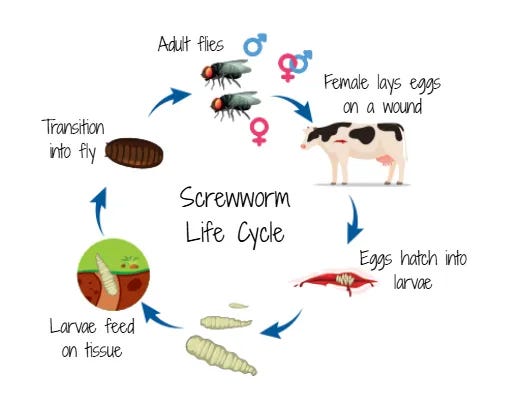
New World screwworm (NWS) is a parasitic fly that was fully eradicated from the U.S. in 1966. It lays eggs in the open wounds of warm-blooded animals. When the eggs hatch, NWS larvae burrow into living flesh. It’s exactly as bad as it sounds, and is fatal if untreated.
How did we keep it out?
Starting in the late 1950s, scientists used the Sterile Insect Technique (SIT): mass-producing sterile males and releasing them to outcompete wild males, collapsing the fly population. It works because female flies mate only once.
Eradication moved down country by country from the U.S through Mexico and Central America over decades, eventually pushing NWS all the way to the Darién Gap in Panama (a remote landbridge of dense, mountainous rainforest). The U.S. and Panama maintained a binational barrier there, dropping roughly 20 million sterilized flies across six flights per week. For decades, it held.
But, for the past few years, it’s been crawling back up, and now, as predicted, to the U.S.
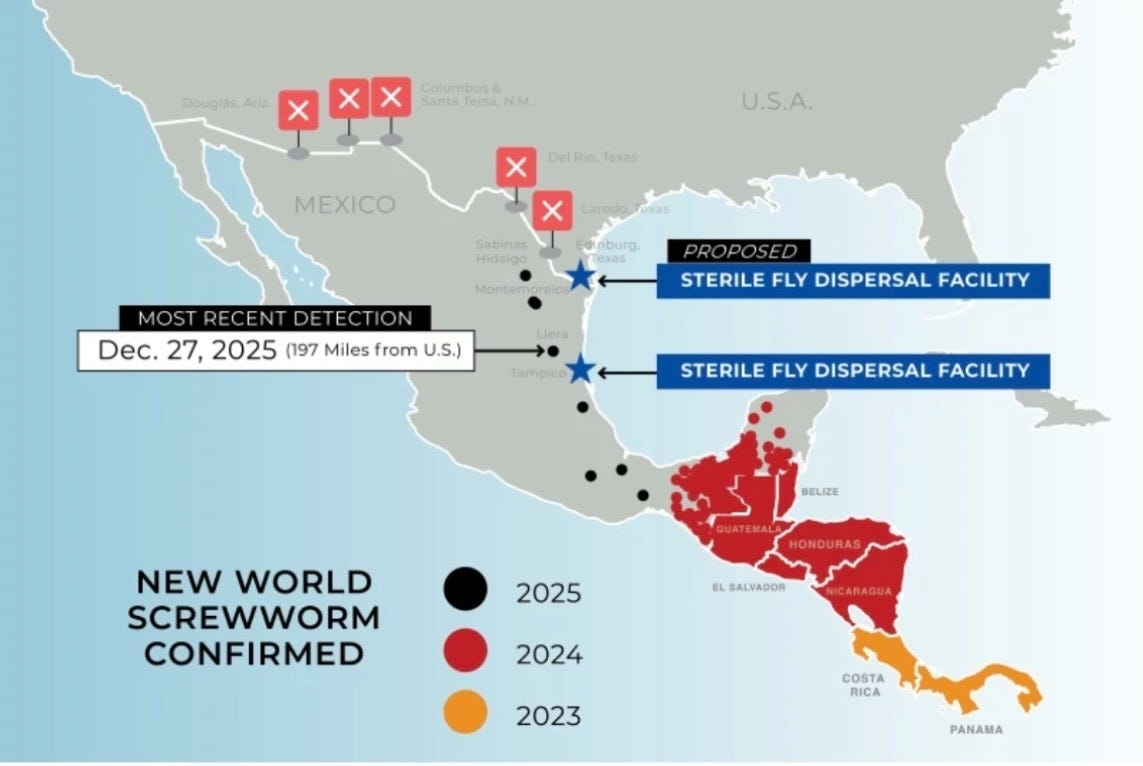
Why is it back?
A combination of factors:
Cattle smuggling. NWS detections in Panama spiked from 25 cases per year to more than 6,500 in 2023, driven largely by cattle movement outside sterile fly zones.
U.S. federal funding cuts. In early 2025, roughly 15,000 USDA positions were eliminated, and a USAID-funded monitoring project was terminated. Warnings passed as the pest moved north through Mexico.
Loss of expertise. In many countries, veteran veterinary entomologists have retired without replacements, taking decades of specialized knowledge with them.
Why does this matter?
NWS spreads fast. A single female lays 200 to 300 eggs per clutch every three to seven days, up to 15 clutches in her lifetime. Eggs hatch within 24 hours; larvae feed for up to 7 days.
Human cases are rare and treatable when caught early. The most recent U.S. case was a traveler who returned from El Salvador last year and recovered. Pets can also be affected.
The bigger concern is the food system. Health and the economy are tightly linked. A 1976 Texas outbreak, a spillover from Mexico, affected 1.8 million livestock. A comparable outbreak today could cost Texas alone $1.8 billion, with losses across NWS’s historic range potentially exceeding $10.6 billion per year, and over $100 billion in broader U.S. livestock economic activity is at stake.
How do we stop it?
Same as before: SIT. Mexico is refurbishing retired rearing facilities to resume sterile fly production by summer 2026. A new U.S. facility in Texas will produce up to 300 million sterile flies per week, though experts estimate 400 to 500 million will be needed for full eradication. Ramping to capacity could take 18 months to two years. Panama is sending SIT males to the U.S. in the meantime.
What this means for you
The biggest concern is livestock, particularly cattle. Here are some tips to keep them healthy. To everyone else, the beef you eat is still safe.
Stray dogs and wildlife are also at risk; pets can be exposed too, but really only in agricultural areas. Ensure pets are on flea & tick prevention from the FDA-approved list, as products containing afoxolaner (dogs) or esafoxolaner (cats) can prevent NWS infection.
For people, risk is not uniform. Agricultural workers in the Southern states, particularly those with open wounds, sores, or skin breaks, are the most vulnerable, as flies are attracted to any open wound.
For everyone else, risk remains very low.
Good news
As always, ending on a lighter note:
Melinda French Gates pledged $215 million to women’s health. Specifically, expanding contraceptive access, maternal care, and menopause research globally, pushing her total investment in women’s health past $600 million over the past two years.
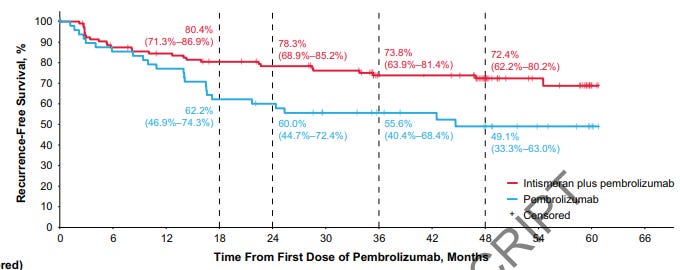
An experimental personalized skin cancer vaccine cut the risk of melanoma returning or causing death by 49% after five years when used in combination with immunotherapy. The vaccine is custom-built for each patient using genetic information from their own tumor, teaching the immune system to recognize and attack it. The vaccine still has a while to go through clinical trials, but this is welcome news given the increasing skin cancer rates.
Inhaled insulin approved for kids with diabetes. The FDA approved inhaled insulin (Afrezza) for children ages 6 and older with diabetes. This is the first needle-free insulin option for pediatric patients in over 100 years. It’s a mealtime insulin delivered via a small portable inhaler, replacing the multiple daily injections kids currently need at meals. Pediatric patients and parents of younger children reported greater treatment satisfaction.
Bottom line
Lots of people and animals are moving, and with them, diseases. We’re keeping an eye on it all and will keep you informed.
Love, YLE







.jpg)














.jpg)