------------------------------------
Threats to public health at every angle
"This month marks the fifth anniversary of the Covid-19 pandemic. Anniversaries are meant for reflection, a moment to take stock, have honest conversations, and apply lessons learned.
"But this is not just any anniversary. Instead of an opportunity to evolve and press forward, public health is in survival mode. It’s being actively threatened from every angle—workforce, infrastructure, discovery, and services for infectious and chronic diseases—driven by priority shifts, pandemic revisionism, political retribution, and (dare I say it) some necessity. This is a dark moment for the field.
"It’s also a dark moment for the American people who bear the consequences of broken systems—sky-high health care costs, high chronic disease rates, mounting fears that we’re completely unprepared for the next pandemic, and a fractured information landscape that forces them to crowdsource health advice on social media.
"It’s frustrating. It’s disheartening. It’s exhausting. And it’s dangerous.
The Covid-19 aftermath is real
"This moment isn’t just about public health. It’s part of a broader reckoning with trust, authority, and expertise. But the timing—just years after a global pandemic—is no coincidence.
"This week, an $11 billion cut slashed local and state public health infrastructure. With literally a one-day notice. What does this mean to you? Turns out, a lot:
Want a modernized system to check your immunizations instead of digging through old records? Public health can no longer upgrade immunization information systems.
Want your mayor to save money and lives by addressing the opioid epidemic? Public health can no longer upgrade disease surveillance and reporting.
Want faster blood test results? Public health can no longer carry out major lab renovations and modernization.
Want to better track measles to protect your family? Public health can no longer conduct wastewater testing.
Want your grandma in a nursing home to live a long, healthy life? Public health must discontinue infection control education for nursing homes.
"The media and political narratives frame these cuts as simply rolling back Covid-19 spending. Yes, the funding was allocated in response to the pandemic, but it was used to address long-standing vulnerabilities—issues that affect every public health topic, not just Covid-19. Public health is inherently crosscutting: Strengthening one area strengthens the whole system.
"Other things that have happened just this week include:
Workforce cuts, including 10,000 jobs (1 in 8) at Health and Human Services.
mRNA vaccine technology is being questioned despite its revolutionary impact on medicine.
Long covid research shut down, which was discovering pathways and treatments for chronic fatigue syndrome in general.
Five top CDC officials resigned, including the Director of Communications.
"This is the latest in a long pattern, including sidelining scientific advancements and canceling global health cooperation to make us safer in the U.S.
The dangers of pandemic revisionism
"Fueling the dismantling of our public health infrastructure is pandemic revisionism—the rewriting of history from the comfortable vantage point of 2025, where we now enjoy the benefits of immunity, scientific knowledge, and hindsight.
"Two years ago, I warned about this on The Ezra Klein Show. And here we are still.
"Just last week, The Daily podcast gave political scientists 45 minutes to argue that non-pharmaceutical interventions—lockdowns, masks, quarantines—didn’t work or, worse, were deliberately implemented by public health officials despite knowing better. This narrative is far from the truth. What’s missing is nuance: We need deep, holistic evaluations of where, why, and how policies work to move in the right direction.
"(To their credit, the two guests have agreed to come on our podcast, America Dissected, for a much-needed back-and-forth conversation, which I appreciate.)
"Consider these pivotal questions that challenge revisionist thinking:
If lockdowns don’t work, why did they succeed in New Zealand and Australia?
If masks are useless, why did flu nearly disappear?
If quarantines are ineffective, should we stop using them for measles?
"These interventions are not relics of Covid—they are the same tools we rely on today for bird flu, measles, and future outbreaks. Yet, we see alarming examples like Florida’s approach to measles in schools, which fundamentally undermines proven public health strategies.
"Let’s be crystal clear: In the first year of the pandemic, we faced a crisis with literally no vaccine, no treatment, terrible diagnostics, no surveillance system, and no federal plan. Outbreaks were widespread, hospitals were overwhelmed, and people were dying. This is not hyperbole—this was our reality.
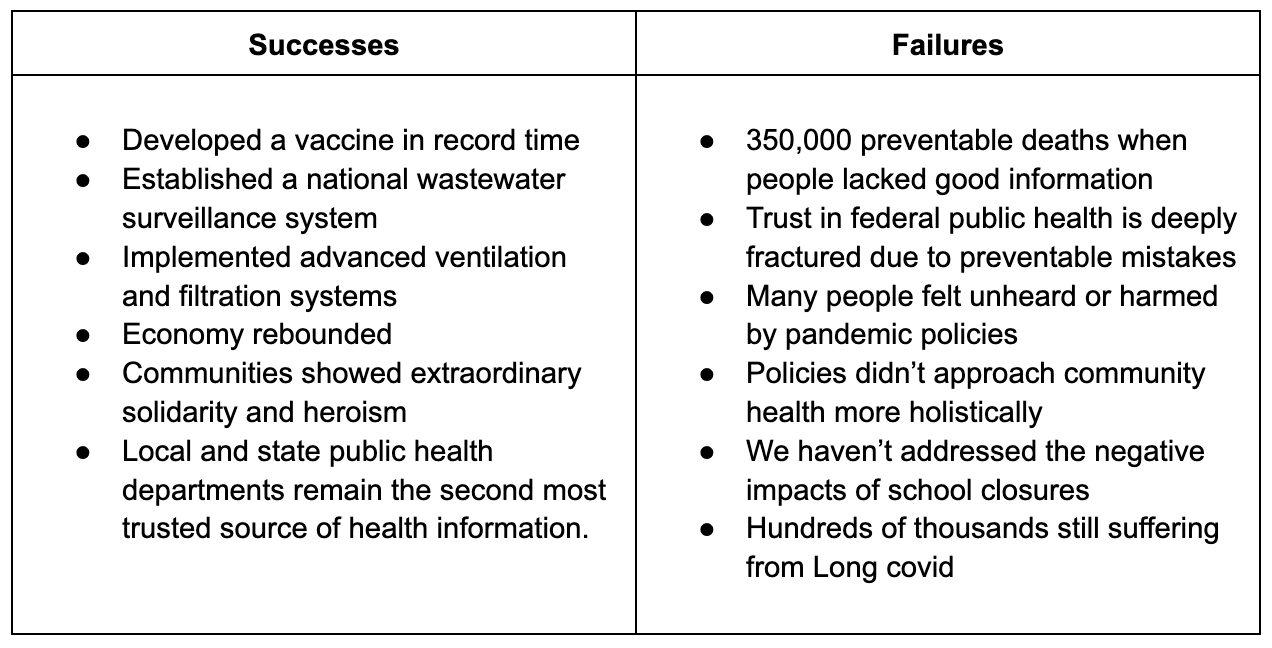
"We must be able to hold two truths: 1. Mistakes were made. 2. Public health demonstrated remarkable resilience. Revisionist narratives often erase the second truth.
"Public health has always been underfunded and understaffed—a system not set up to succeed. And we are doing nothing to fix that infrastructure now.
Chronic vs. infectious disease battle
"Covid-19 also brought in its wake the false pretense that public health doesn’t focus on chronic health, nutrition, or other key issues that Americans care deeply about. These hot takes are dangerously misleading.
"The U.S. has entire centers of research and practice dedicated to diabetes, cancer, Alzheimer’s, chronic disease, mental health, etc. The 22 Healthy People 2030 goals for public health prevention focus more on chronic diseases than infectious diseases. (Go here for progress towards each.) For decades, people have been studying and implementing best practices. That progress has been stalled because of policy blocks. The last big effort was during the Obama administration, which was met with fierce political opposition.
"So don’t be tricked: these cuts today dramatically impact chronic disease, too:
Sidelining scientific advancements, like in diabetes and cancer research.
Cutting USDA programs that support healthy eating at schools and local farmers.
$1 billion cut to substance use and mental health services.
Abruptly halting training for future cohorts of public servants.
"As I’ve written before, there are smart, tactful ways to remove bloat. But what we are seeing isn’t careful reform. This is a sledgehammer approach with little regard for the real-world consequences.
Cycle of panic and neglect
"This is what we in public health call the cycle of panic and neglect—a surge of support during crises that drives rapid investment, attention, and action, only to fade once the immediate threat passes, leaving systemic problems unresolved time and again.
"It isn’t new, but this is the most extreme we’ve seen. The “Sisyphean Cycle” was coined after Greek mythology in which Sisyphus— a “trickster who receives eternal punishment for trying to cheat death”—was condemned by the gods to roll a boulder up a steep hill for eternity. Every time he reached the top of the hill, the rock rolled back down to the bottom, forcing him to start all over again.
"We are actively watching the boulder roll back down the hill.
Where do we go from here?
"There is very little energy right now—for hard conversations, for mobilization, and for an already burned-out workforce being asked to do more with less. The only thing holding the public health system together is the unwavering workforce commitment with one clear mission: healthier communities. But how much longer can that last? A poll this week found 75% of scientists are considering leaving their jobs.
"It’s hard to see the path forward. The current leadership has a lot of explaining to do about how this is America first and how this makes us healthier.
"But we must remember: there is always a long game.
"Public health infrastructure has always gone beyond government programs. While these are vital—healthy societies invest in direct public health services—we also see another layer of protection when government falls short. The safety net of community leadership, the countless hidden acts of service and advocacy, and the resilience of those who continue to fight for health at the local and federal level.
"In a democracy, an educated public is the primary means to correct government errors. (Cough, cough, YLE.) We don’t yet know the full trajectory of this moment. But we do know that, by and large, Americans value the people who protect their health. Trust in public health may be battered, but it is not broken: the top two trusted sources of health information are doctors and public health departments. 88% of Americans still believe in routine vaccinations, grassroots efforts are mobilizing, and bipartisan support is emerging against big lobby groups that undermine health. And when policies start impacting lives in tangible ways, the public will take notice.
"This moment is dark. It may be for a while. But it’s not the end. After all the pieces fall, I’m hopeful that there will be an opportunity to rebuild something stronger, more responsive, and less vulnerable to the forces that seek to undermine it.
Bottom line
"This Covid-19 anniversary is different. It hasn’t been about looking back to learn for the future—it’s been about surviving the present and preventing, with all our might, the boulder from rolling back down the hill.
"One thing is certain: we cannot go back. The stakes are too high to forget. The lessons are too important to dismiss.
"Love, YLE"
A huge thank you to Dr. Matt Willis for his feedback on a number of drafts.
Your Local Epidemiologist (YLE)
is founded and operated by Dr. Katelyn Jetelina, MPH PhD—an
epidemiologist, wife, and mom of two little girls. Dr. Jetelina is also a
senior scientific consultant to a number of non-profit organizations.
YLE reaches over 340,000 people in over 132 countries with one goal:
“Translate” the ever-evolving public health science so that people will
be well-equipped to make evidence-based decisions.















.jpg)
No comments:
Post a Comment